Three months ago, a surgeon at Liverpool Heart and Chest hospital took a saw, ripped through my sternum, levered open my ribcage, cut into the aorta of my still-beating heart and stitched in a vein from my leg. The long, brutal operation was a great success. But it knocked me out and left me unable to walk more than a few paces.
As I recovered, I got to asking how had I got into this mess. I had always, I thought, kept pretty fit: I could happily walk all day in the hills, chop wood, play cricket and dig deep. I ate good food and loved exercise. So what else was there in my lifestyle that could have led to heart disease, Britain’s biggest killer?
The doctors routinely blamed my smoking for 20 years, though I had started late and given up more than 11 years ago. But there was also the fact that I had grown up, and then worked, in some of the most heavily polluted places in the world: Birmingham, Sunderland, Dhaka, Accra, Lagos, Jakarta, London and Paris, to name a few. Was it those lungfuls of foul air in Bangladesh, or in Birmingham in the 1960s? Was it covering smogs and pollution in Russia for the Guardian? Could heart disease be the price of living in a modern city?
Appreciation that city life is not just fast, but possibly dangerous, dawned slowly. When young, I could easily ignore the stinging eyes, acrid smell and need to spit after walking or cycling for a few minutes in a busy street. The suspicion that air could be a killer only started seriously with the wheezing I experienced long after I had quit smoking, when climbing a mountain became harder and the pauses for breath longer. I was shocked, in 2009, to be diagnosed with angina. But I was knocked out when last year I was told I needed a heart bypass. That happened only to people who were really ill, didn’t it?
I worked in some of the most polluted places in the world. Could heart disease be the price of living in a modern city?
“See it as a precaution. Statistically, you’ll live longer,” said my cardiologist. “If you don’t have it, you can expect a heart attack any time.”
In the worrisome months following the diagnosis and before the operation, I delved into the scientific literature. The links between air pollution and heart disease, only a generation ago uncertain, were now robust. Paper after paper showed how long-term exposure to air pollutants was now linked to high blood pressure, strokes and heart conditions like mine.
But how much of my heart disease was self-inflicted and how much imposed? As people increasingly gave up cigarettes and heavy industry migrated to China and the east, were Europeans becoming more exposed to other sorts of air pollution? Were the streets of London or Paris more dangerous now than in the past?
I asked Fintan Hurley, science director at the Institute of Occupational Medicine (IOM) in Edinburgh. “I think of air pollution as one risk factor among many that increases the risk of earlier death,” he says. “Everybody is exposed. And largely it’s involuntary. Active cigarette smoking has at least the appearance of being a choice. A person may have some choices about how much air pollution they experience, but basically, it’s a risk factor imposed by society as a whole to which an individual contributes.”
He and Frank Kelly, who chairs the Committee on the Medical Aspects of Air Pollution, shocked the British government in 2010, when they stated that air pollution caused the premature deaths of 29,000 people a year in Britain – second only to smoking. Some researchers believe the mortality rate could actually be up to twice as high. So how have we reached this point? And why isn’t more being done?
I started to look for answers in the place where modern air pollution could be said to have really got going: Coatbridge, 10 miles east of Glasgow. In Victorian times, this was Britain’s – maybe the world’s – most polluted town. Its 300 coalmines, 50 steel blast furnaces and innumerable factory chimneys pumped out hundreds of tonnes of soot, sulphur and noxious vapours every day.
Today, the heavy industry has long gone and the once-dark Coatbridge air is cleaner than in most other British towns. Indeed, at 10.40 on a bright April morning, on the site of an old iron smelter in what is now the Summerlee museum of Scottish industrial life, a monitor borrowed from the IOM barely registered Britain’s two main air pollutants – the toxic gas called nitrogen dioxide (NO2) and the tiny particles of soot, or dust, called PM2.5s.
Kerry Garvie, whose father was a miner in nearby Bedlay colliery, recalls how her mother struggled to keep anything clean, how her Uncle John had breathing problems and how her clothes always got black. For Garvie’s relatives, air pollution was a fact of life, and life was often short. “It is what they lived with and what they knew,” she says.
‘Cigarette smoking has at least the appearance of choice. Air pollution is a risk factor imposed by society as a whole’
Fintan Hurley, Institute of Occupational Medicine
But do we know better now? Ten miles west of Coatbridge, Glasgow city centre was that day, as usual, snarled with traffic. Wherever I walked with Emelia Hanna, Friends of the Earth Scotland’s air pollution campaigner, the monitor read five or more times higher than in Coatbridge. The fine particles peaked in the taxi rank outside Queen Street railway station; the nitrogen dioxide count soared way over the European legal limit near main roads. Glasgow has tighter pollution laws than England and Wales, but is far and away Scotland’s most toxic town. “No wonder,” Hanna says. “It is ringed by motorways, served by hundreds of old diesel buses, its lines of cabs keep their engines running all day.”
According to government figures, air pollution is responsible for more than 300 deaths a year in Glasgow. “Most people here know someone affected by asthma, heart disease or lung problems,” Hanna says. “It affects children and people on lower incomes worst.”
***
Neighbouring Coatbridge and Glasgow show how air pollution in Britain has changed in just a few generations. The coal and wood smoke that belched from Britain’s factories and hearths may have vastly reduced, but it has been replaced by a toxic soup of nitrogen oxide gases and minute particles of unburned carbon and chemicals, produced by vehicles and fossil fuel-burning central-heating systems. Instead of pollution being concentrated in old industrial centres such as Sunderland, Widnes or Newport, the fumes are now worst in congested cities such as London, Birmingham, Leeds and Sheffield.
The difference between now and 100 years ago, says Kelly, who is director of the environmental research group at King’s College, London, is that today’s air pollutants are largely invisible and odourless, and are obvious only when dust is occasionally swept up from the Sahara or when traffic and industrial fumes get trapped on sunny days and a dull orange-grey smog develops. “These acute events result in thousands of extra hospital admissions and breathing complaints, but they are relatively rare,” he says. “They come on top of the chronic air pollution that all British cities experience every day from heavy traffic. Some pollutants may indeed have disappeared since the infamous smogs of the 1950s, but people have an increasing level of other complaints, such as asthma attacks, cardiovascular and breathing problems.”
Kelly’s office, housed on the upper floors of a drab 1960s building in south London, is the world’s largest centre of public research into the medical effects of air pollution. He and other scientists working here advise not just the UK government but the World Health Organisation and the most polluted countries in the world, such as China and India. Kelly and his colleagues now see air pollution spreading as populations and cities burgeon and, above all, as the car becomes ubiquitous. In 1950, there were around 4m cars in Britain and 35m in the world. Now, we have 28m and there are more than 750m worldwide, along with 200m vans and lorries.
Could I really pin my own heart disease on the air I have breathed, as well as the smoke I have voluntarily inhaled? Certainly, says Ian Mudway, Kelly’s colleague and a lecturer in respiratory toxicology, whose research shows that children’s health is greatly affected by air pollution from a very early age.
I first met Mudway at a residents’ meeting in the London borough of Tower Hamlets. He had been researching the lung capacity of children living near busy east London streets, and was telling his audience how the health of their communities would inevitably deteriorate if a new Thames road bridge or major tunnel was allowed to bring thousands of extra cars a day into the East End. “We have high-density housing here, slap-bang next to major roads,” he told the audience. “People still don’t see air pollution as a big issue. They understand that you die from alcohol or obesity, but air pollution doesn’t have that risk factor in people’s imagination. Yet it’s a killer.”
The more researchers like Mudway have looked at people’s long-term exposure to air pollution, the worse the picture gets. The cautious International Agency for Research on Cancer suspected that PM2.5s were carcinogenic to humans back in 1988, but only in 2013 could it definitely say they were a cause of lung cancer. The most recent World Health Organisation data suggests there were 233,000 deaths from lung cancer caused by air pollution around the world in 2011. Meanwhile, a study from the University of Washington in the US cites 3.4m deaths from outdoor air pollution in 2010 – 400,000 more than in 1990.
For everyone who dies, there are many more hospitalised or who have impaired health
Ian Mudway, lecturer in respiratory toxicology
Adding the effects of indoor pollution, mostly from cooking fires in the developing world, brings the global death toll to 7m a year, according to the World Health Organisation. In short, air pollution is now officially the world’s biggest environmental cause of premature death – second only to smoking and the equivalent of alcohol and obesity combined in the UK and, in 2013, causing more deaths worldwide than Aids and malaria.
But where are the victims? No postmortem states air pollution to be a primary cause of death, and few people take a day off work because of it. Yet we now know that PM2.5s, which get deep into the lungs and bloodstream from exhaust fumes, can greatly worsen respiratory and heart conditions such as my own, trigger heart attacks and lead to brain damage, cancers, even nerve, liver and kidney diseases. “For everyone who dies, there are many more hospitalised or who have impaired health,” Mudway says. “Prolonged exposure to elevated [particulate pollution levels] is associated with significant life-shortening and poor respiratory health. Acute episodes can precipitate death.”
***
Mal Chadwick is a young, fit cyclist, but when he arrived in London from York five years ago, he found himself wheezing. He cycles around 40 miles a week in the city, and his doctor has diagnosed asthma, almost certainly aggravated by air pollution. “The air quality of the two cities is noticeably different,” Chadwick says. “When you bike in London, you get it full in the face.”
He uses an inhaler three or four times a week, but the pollution is worse in autumn and spring, when the temperatures can go quickly from cold to warm, and when the traffic is heavy. “I used to take the main roads,” he says. “Now I only go on the back routes.”
Charlotte Dalton, 18, lives close to Junction 1 on the M3 in west London and suffers from bronchitis, also caused or aggravated by air pollution. “I have lived on Staines Road West for 16 years,” she tells me. “Whenever the windows are opened, car fumes fill the house. When I suffer, it hurts to cough and it’s painful to talk. I’ve had to take a week off school to recover at times.”
“I’m relying heavily on meds today,” a colleague tells me. “People on the tube were giving me that wary, angry look they give constant coughers – I felt as if I should be wearing a sign that says, ‘It’s not contagious, it’s asthma.’ ”
“Diesel is the real villain,” says Simon Birkett, a former City banker who gave up his job to set up an air action group in 2007. Petrol fumes may be bad for health, but diesel engines pump out nearly 65% more particulate pollution and nearly 20 times as much nitrogen oxide gases as petrol cars over their lifetimes. Moreover, their particulates are often smaller and more likely to get into the bloodstream.
“What is extraordinary,” Birkett says, “is that, even though the European commission, national governments and the car industry know how dangerous diesel is, together they incentivised it and deliberately engineered a massive switch away from petrol – without any public debate.” History, he says, may show that the rise in heart disease and other illnesses now linked to air pollution has coincided with the increase in awareness of another environmental problem:climate change. And that a botched attempt to address the one has exacerbated the other.
In the 1990s, climate change was rising fast up the international agenda and, following the 1997 signing of the Kyoto protocol, rich countries were legally obliged to reduce emissions by an average of 8% over 15 years. But while Japan, China and the US chose to back research into low-emission hybrid, petrol and electric vehicles, Europe prioritised a mass public switch to diesel, announcing that it not only gave 15-20% better mileage to the gallon, but emitted around 13-17% less carbon dioxide, the main climate-changing gas. The motor industry, governments and the green lobby reasoned that it would be one of the cheapest and easiest ways to tackle climate change.
Was my health, and that of millions of others, cynically traded off against the urgency to control climate emissions?
By any measure, the transformation of the European car fleet from almost entirely petrol to predominantly diesel was rapid and remarkable. Britain, along with Germany, France and Italy, offered subsidies and sweeteners to persuade car makers and the public to buy diesel. Key to the change was the 1998 Acea voluntary agreement between the European commission and all European car makers, backed strongly by then EU transport commissioner Neil Kinnock and UK environment secretary John Prescott. This committed all car makers selling in Europe to reduce their average CO2 emissions for new passenger cars by 25% over 10 years. It was practically an order to switch to diesel.
At the demand of industry, Britain and other countries kept the diesel price below that of petrol, and penalised petrol vehicles with higher road tax bands. Emission standards for MOTs were linked to CO2, and the car and oil industries were set new targets for diesel adoption.
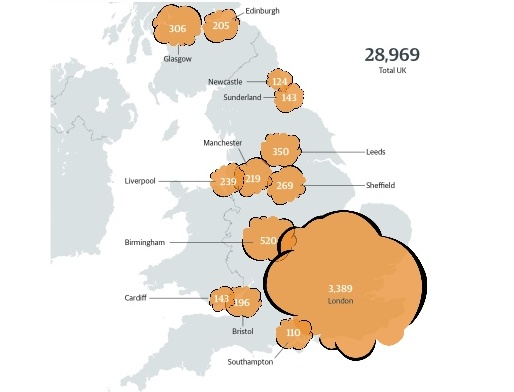
Deaths attributed to long-term exposure to air pollution in 2012. Source: Public Health England 2014
The results were dramatic. From being a quirky consumer choice, diesel went mainstream in the world’s biggest car market. Its share in the UK rose from less than 10% in 1995 to over 50% in 2012. Most taxis and buses are now diesel. With more than 1m new diesels now sold a year, and 9m on its roads, Britain has one of the largest diesel car fleets in the world.
The picture is similar across Europe: more than 55% of all new European car registrations are now diesel, and the region has around 100m diesels, compared with just a few million in the US, China and Japan. The diesel fuel market has grown so fast that the EU now imports much of its diesel and exports petrol to the US. Britain is expected to have to triple its imports over the next 10 years.
So was my health and that of millions of others cynically traded off against the urgency to control climate emissions? Those working in the UK government in the 1990s recall how climate change trumped any objections from scientists, or from the few people who understood the health implications of a major switch to diesel.
One who did understand was David Fisk, chief scientist and policy director in the departments of both the environment and transport in the 1990s. He recalls that there was “concern” in government when it was proposed that diesel be backed over petrol. “The motor manufacturers made a démarche to the department of the environment, showing that a major switch to diesels would lead to a substantial drop in CO2 emissions. Air quality division saw straight away that there was a problem,” he says. “It was hard to see how anyone could construct a trade-off algorithm that made much sense. The solution was to create the national system of air quality standards.”
Former Greenpeace chief Stephen Tindale, who was working on air pollution at the same time, in the department of the environment, remembers a battle between environment and air pollution divisions, but no public debate about health. “British politicians have always been poor on air quality,” Tindale says. “It was just not on the political agenda in late 1990s. In 1997, Labour’s policy was for a 20% cut in CO2 emissions by 2020. Tony Blair wasn’t obsessed with climate at that point, but he saw the political and soundbite advantage. The department of health was dozy, with Frank Dobson and then David Blunkett in charge.”
A very senior civil servant, now retired, who worked in the department and has asked not to be named, said that cost-benefit studies of a switch to diesel were done, but climate change was “the new kid on the block” and long-term projections of comparative technologies were not perfect. “I recall all the discussions had the health issue as a significant factor,” he says. “We did not sleepwalk into this. To be totally reductionist, you are talking about killing people today rather than saving lives tomorrow. Occasionally, we had to say we were living in a different political world and everyone had to swallow hard.”
Former environment minister Barry Gardiner has admitted fault, telling Channel 4’s Dispatches TV programme last year that it was the “wrong decision” to incentivise the purchase of diesel vehicles. But Michael Meacher, environment minister at the time, says he cannot recall ever being consulted on the proposed switch to diesel by his civil servants: “If it had been a question of a trade-off between carbon emissions and health, much as I would have wanted to reduce climate emissions, the medical effects would have trumped it. I would have been keen to see a major reduction in [carbon] emissions, but I would not have wanted that to be at the price of lives.”
Frank Kelly now thinks that thousands of people – many with conditions like mine – may be dying prematurely in Britain each year because of the decision to cut carbon emissions at the expense of air pollution, without exploring alternatives. Even worse, it now emerges that Britain and Europe may have only marginally reduced their carbon emissions from transport by switching to diesel, and possibly did not reduce global warming levels at all. Over the last few years, scientists have found that the fine particles emitted by diesel engines play a far bigger role in global warming than many previously thought. The smallest particles, known as “black carbon”, trap heat in the atmosphere and are now thought by some to be second only to carbon dioxide as a driver of global warming.
Back in London, I went to Oxford Street, last year cited by King’s College air researcher David Carslaw to be the most polluted street in the world, a “diesel corridor” used by thousands of buses a day. According to Carslaw, it had some of the highest concentrations of NO2 gas measured in any street in the world.London mayor Boris Johnson was offended by this suggestion, responding furiously that it was “bollocks”, but no one, Carslaw says, has disproved it. Since then, Johnson has promised the world’s first ultra-low emission zone from 2020, and has launched a campaign to warn parents to choose less polluting routes to take their children to school.
A toddler was given a carbon monitor: most of the pollution she breathed in came in two hours, going to and from nursery
Outside Selfridges, I met Marie Bristow from Bexley, who had taken a day off work to go shopping. It was a hot day, she’d come up by bus and train and London’s air was officially “good quality”. “I only come when I have to,” she says. “No one likes the air here. It’s the buses, isn’t it? I go back in the evening and it takes me hours to recover. My sister worked here for years and wheezed all the time.”
The NO2 may be bad on Oxford Street, but it’s the fine particles in diesel fumes that concern researchers most. Carslaw’s colleague Ben Barratt last year gave portable carbon monitors and GPS watches to seven south London residents, including a pensioner, a cycle courier, an office worker, an ambulance driver, a school pupil and a toddler. He then measured the greatly varying amounts of pollution the volunteers breathed in as they went about their days. Over a 24-hour period, the ambulance driver was exposed to the highest levels, because the traffic exhaust was entering the cab of his vehicle; the cyclist was exposed to half that, and the lowest levels were inside the office worker’s building. Most of the pollution that a toddler breathed occurred in just two hours on the journey to and from her nursery in a pushchair; and the school pupil was exposed to more pollution when travelling on the bus than when walking home along quieter streets. Other studies show that walking and cycling in back streets is better than car travel.
According to Barratt, “This suggests that the exposure to pollution may actually be higher for someone driving a car around busy roads than doing so on a bike. This is a simple message that we can tell people, so we can considerably reduce levels of exposure.”
Crucially, his study showed that particulate pollution varied minute by minute, vehicle by vehicle and street by street. “The way to understand air pollution is to see it as cumulative over a person’s life,” he says. “We know it affects birth weight. A baby born with low birth weight has an increased risk of disease in later life. If he or she goes to a school in a polluted place, their lungs will not develop, which further increases the chances of developing cardiovascular or other diseases later. By the end, the likelihood of air pollution finishing you off is higher.”
Barratt says the chance of dying from smoking cigarettes is about 10 times higher than from air pollution in the UK, “but on a population scale, the risk is just the same”. Those of us walking and cycling along busy streets are “passive smokers of vehicle exhausts”. He recommends real-time pollution apps developed at King’s, so people can get up-to-date information and plan routes across cities. At the moment these only cover London, but they will soon be extended to other cities.
The government, ordered this year by the supreme court to draw up a new UK air-quality plan, has accepted that air pollution costs the economy up to £18bn a year, or a seventh of all NHS spending; but has told Europe that it will not meet legal NO2 limits in London, Birmingham and Leeds for 16 years, and in cities such as Liverpool, Sheffield, Manchester and Glasgow for 10.
“Cracking our air pollution problem is a huge challenge,” says Kelly. “Traffic must be reduced, and we must ensure a cleaner and greener element to what remains on the road. This can be achieved through a number of strategies: an expansion of low emission zones, investment in clean and affordable public transport, a lowering of speed limits, a move back from diesel to petrol, or at least a ban on all diesel vehicles not fitted with a particulate filter.”
***
Now the idea of breathing London’s air seems horrible, and the gusting winds of the Welsh hills taste gloriously clean
So was my heart disease caused by cigarettes, or those lungfuls of dirty air in London, Birmingham and Lagos? It’s impossible to say. Best not to look for one simple answer, concludes Hurley. “Personally, I don’t spend much time wondering whether air pollution initiates the heart disease that later causes earlier death, or whether it accelerates disease initiated by other factors. For me, the main point is that it does increase the risk.”
Three months after my operation, the idea of breathing London’s air seems horrible, and the gusting winds of the high Welsh hills taste gloriously, absurdly clean. I was lucky to have been given another chance by the extraordinary skills of the surgeons and cardiologists. But the hospital wards full of wheezing people with lungs and hearts permanently damaged by lives spent near busy roads tell another story.
via All choked up: did Britain’s dirty air make me dangerously ill? | Global | The Guardian.






















Why do you blame Diesel engines as causing more particulate pollution then modern direct injection petrol engines, that do pollute more then a Diesel car with properly working particulate filter? I didn’t see a suggestion to incentive the use of gas powered cars (CNG and LPG) , which are widely available and emit zero particulate matter.